Senior Product Designer | Enterprise SaaS
NORTH STAR HOSPITAL PILOT
Hidden scheduling rules were causing operational risk across home-health operations
I analyzed 70+ incidents initially triaged as backend bugs. The root cause was not system failures, but invisible scheduling rules.

PROJECT OVERVIEW
Impact
Reduced scheduling validation time by 52%, and invalid scheduling attempts by 25%
Role
Founding product designer.
End-to-end ownership from research to production pilot.
System Challenge
The scheduling engine already handled complex rules (coverage windows, clinician availability, compliance).
However these constraints were invisible in the interface, forcing schedulers to mentally simulate the system.

REFRAMING THE PROBLEM
“This looked like a backend issue,
but it was a product clarity issue.”
Initial triage identified these as backend bugs — a reasonable assumption given the symptoms. I conducted a deeper audit of 70+ incidents and found a different pattern: every case was a constraint communication failure, not a system error. The rules were correct. The interface was hiding them.

To understand the incidents, I mapped the full constraint model behind the scheduling system.

Scheduling decisions were constrained by multiple hidden rules that clinicians could not see in the interface.
CONTEXT
Scheduling decisions depended on rules that were invisible in the interface
Overview
Axle Health is an AI-powered home health scheduling platform that coordinates clinician visits for 3,000+ patients daily across healthcare agencies. Schedulers are responsible for booking visits that must comply with insurance coverage windows, clinician availability limits, visit frequency rules, and compliance constraints — all enforced invisibly by the backend
THE PROBLEM
The system had the right rules but failed to make them visible at the point of decision
This shifted the conversation from 'fix the bug' to 'redesign how constraints are communicated,' and made constraint visibility a first-class design requirement going forward.
01.Schedulers could not see coverage boundaries
Schedulers could not determine whether a visit fell within a valid coverage window.
02.Scheduling decisions lacked full context
Schedulers did not have access to all required inputs when making decisions.
03.Coverage rules had to be mentally calculated
Schedulers manually combined insurance rules with scheduling decisions.

The backend maintained rules, but the interface did not surface them
TURNING POINT
The pivot
The PM initially wanted to focus on form cleanup. The CTO was concerned about engineering scope. I reframed the audit as a product visibility failure — not an engineering problem — and that shifted both of them.
I presented a 70-incident audit to the CEO, PM, and CTO. Every ticket labeled 'backend bug' was actually a constraint communication failure. That reframe shifted the roadmap — from engineering fixes to product visibility as a first-class requirement
HOW I FRAMED THE PROBLEM
This wasn’t a scheduling UI issue
It was a decision-making problem caused by invisible constraints.
I reframed the system around:
-
Making constraints explicit
-
Ensuring consistency across surfaces
-
Supporting reliable decision execution

RESEARCH & SIGNALS
70+ recurring incidents surfaced during peak enrollment periods.
Two systemic signals emerged from the incident analysis:
1 Trust failures
2 Decision friction
These signals pointed to a deeper issue not incorrect rules, but invisible system logic.

Operational signal
OPERATIONAL MENTAL MODEL
“If the system allows it, I assume it’s valid.”
This belief is rational. The product must earn trust by showing boundaries and reasoning at the point of action.
DESIGN CONSTRAINTS
System Constraints in Scheduling
DESIGN PROCESS
From Fragmented Logic to Consistent Decision System
These constraints were invisible in the interface — schedulers had to mentally simulate the system.
-
Coverage windows
→ surfaced as timeline boundaries in the calendar -
Visit frequency limits
→ flagged when approaching limit -
Clinician availability
→ displayed before slot selection -
Compliance constraints
→ shown inline with eligibility status
01 Surface constraints at the moment of decision
→ Coverage windows and eligibility boundaries embedded directly in the calendar view, not hidden in a side panel or external record.
02 Replace manual rule interpretation with system feedback
→ Explored high-density vs. decision-clarity layouts. Tested with 6 schedulers. Chose clarity over configurability after 3/6 found dense layout cognitively overwhelming during time-sensitive decisions.
DESIGN TRADE OFF
Design Trade-off
Information Density vs Decision Clarity
Clinicians needed immediate eligibility clarity. High information density
increased cognitive load.
Design Exploration: To improve prioritized clarity, I explored multiple layout directions balancing calendar density and decision clarity


LEFT - HIGH INFORMATION DENSITY
RIGHT - DECISION CLARITY (FINAL DESIGN)
Pros
• More scheduling variables visible in one view
• Greater flexibility for advanced scheduling
• Detailed calendar configuration possible
Cons
• Schedulers must mentally combine multiple constraints
• Higher cognitive load during scheduling decisions
Pros
• Coverage eligibility is immediately visible
• Reduced manual rule interpretation
• Lower cognitive load for clinicians
Cons
• Less flexibility in manual configuration
Design Decision: We intentionally prioritized decision clarity over information density to support faster and more reliable scheduling decisions.
SOLUTION
The calendar surfaces coverage constraints
directly within the scheduling workflow.

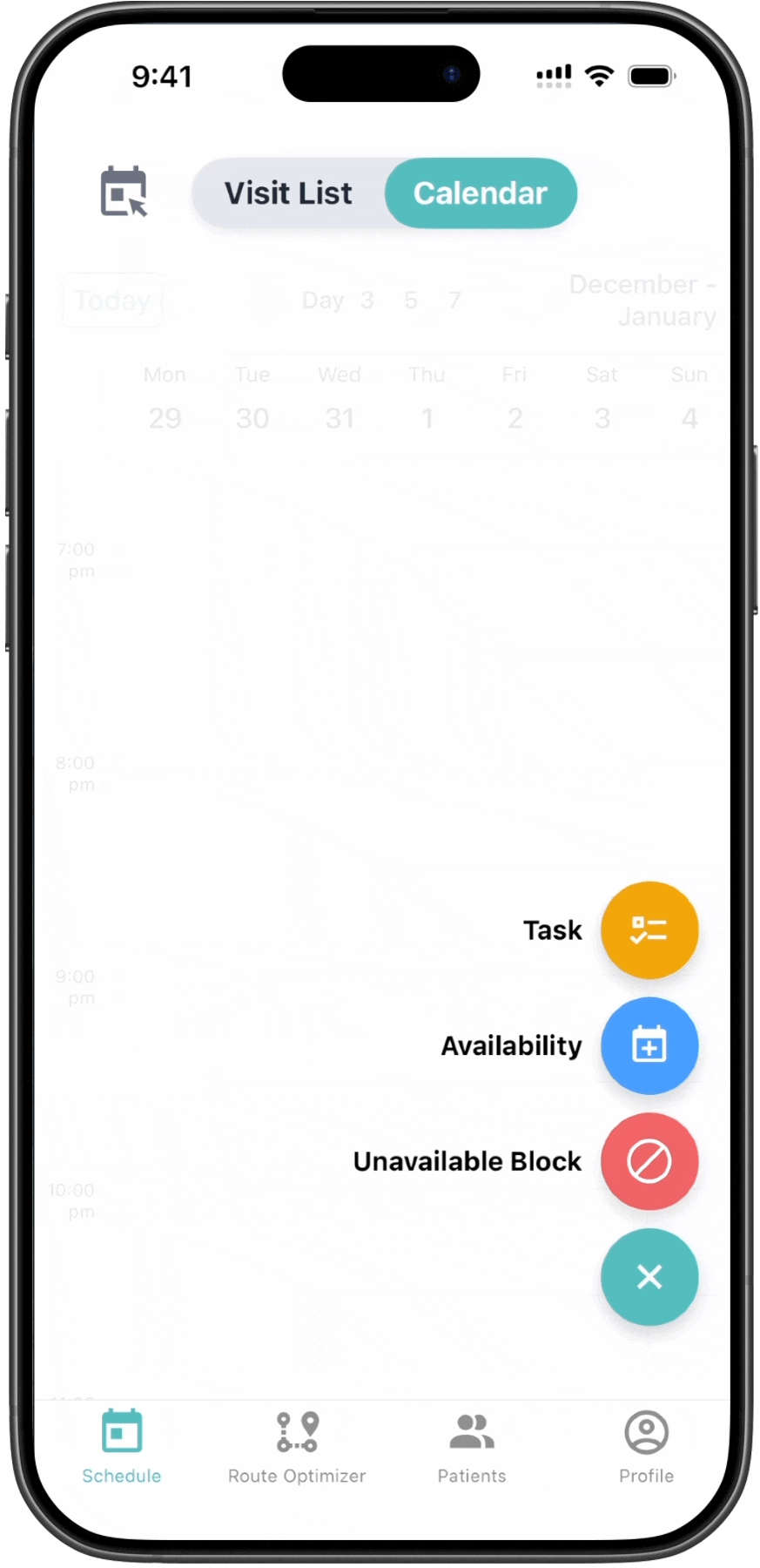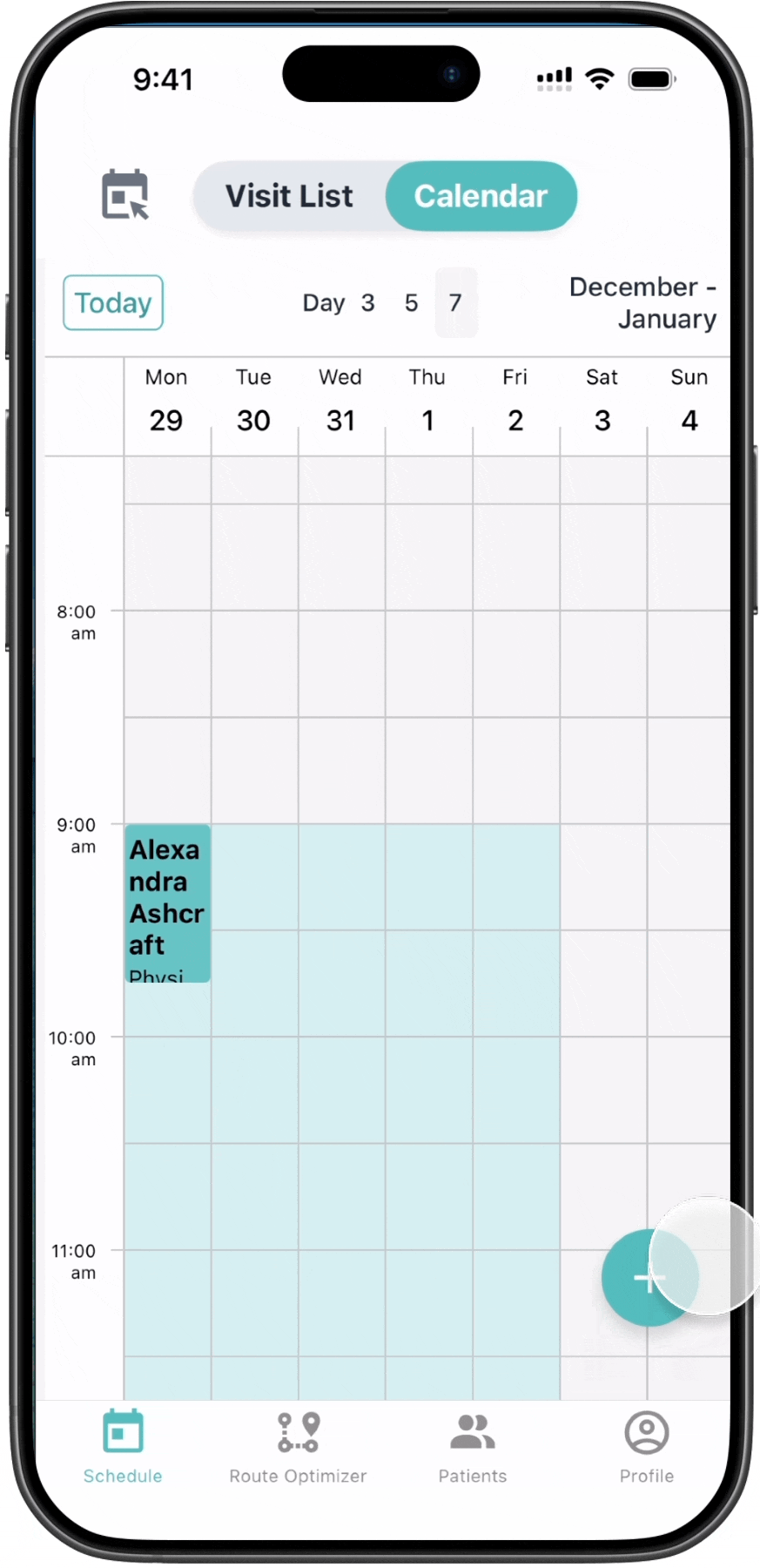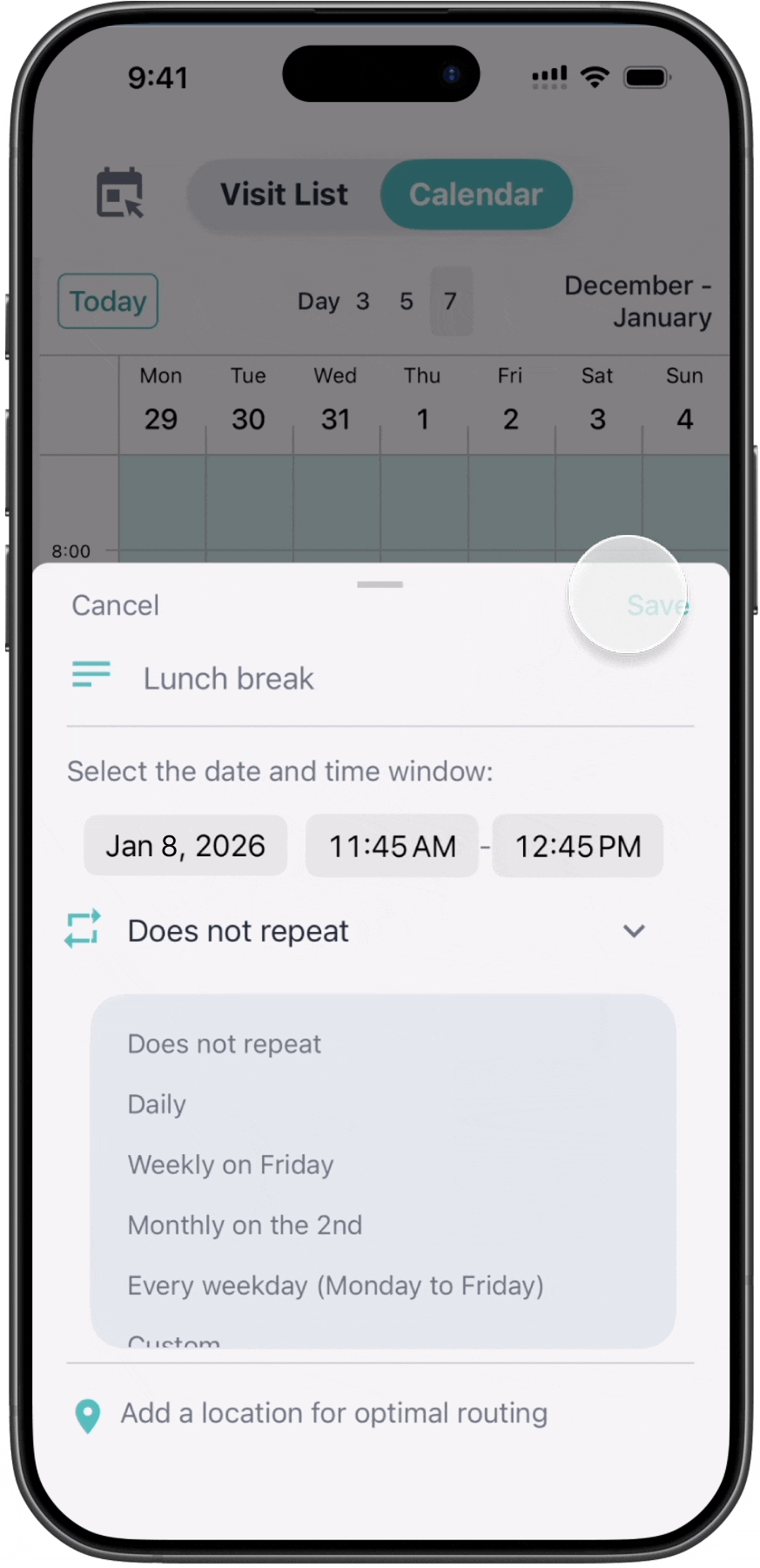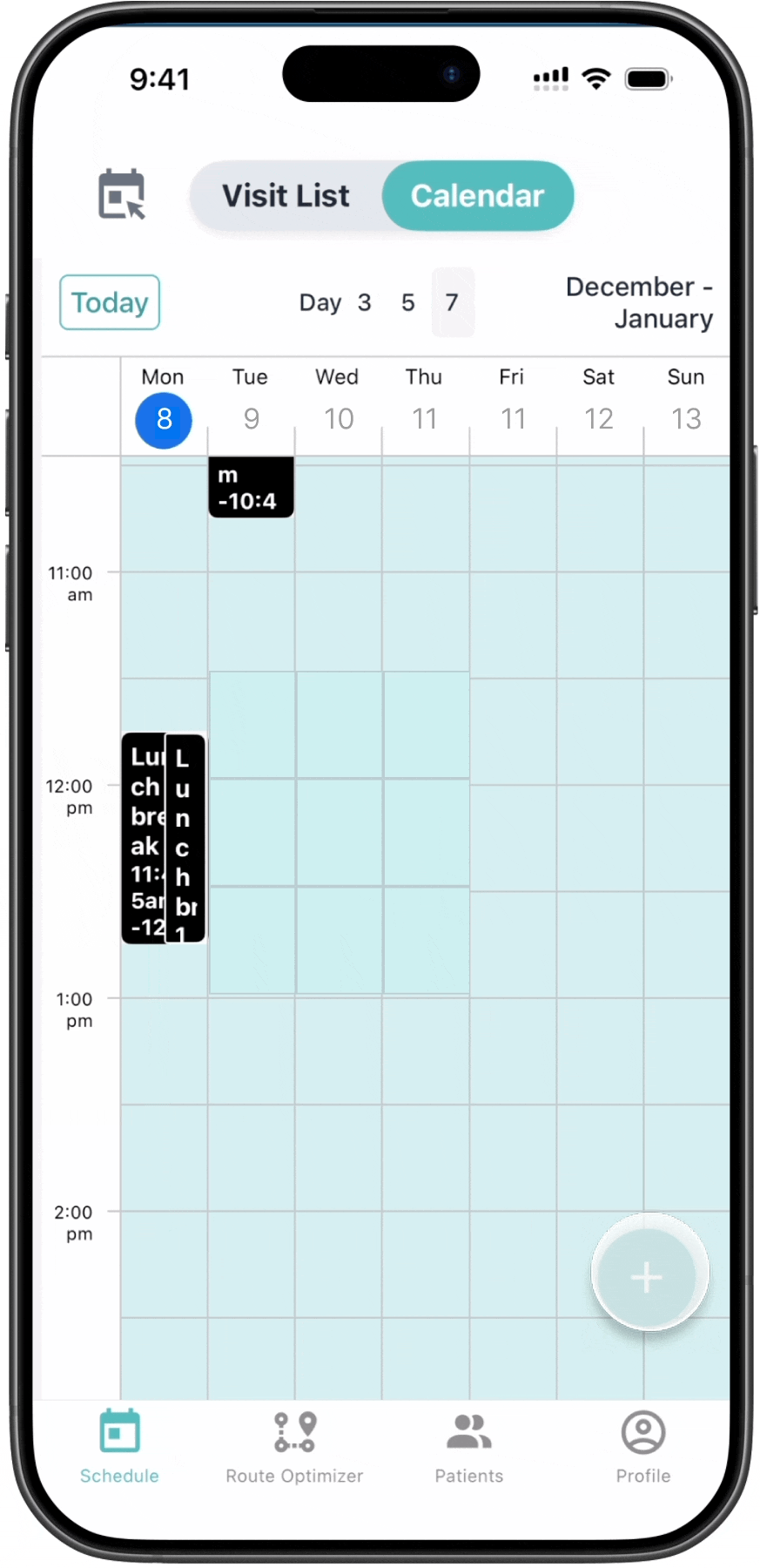
BEFORE
01. Coverage timelines were invisible
Schedulers could not see coverage boundaries while scheduling.

02. Eligibility required manual verification
Schedulers had to check insurance records outside the system.
BEFORE


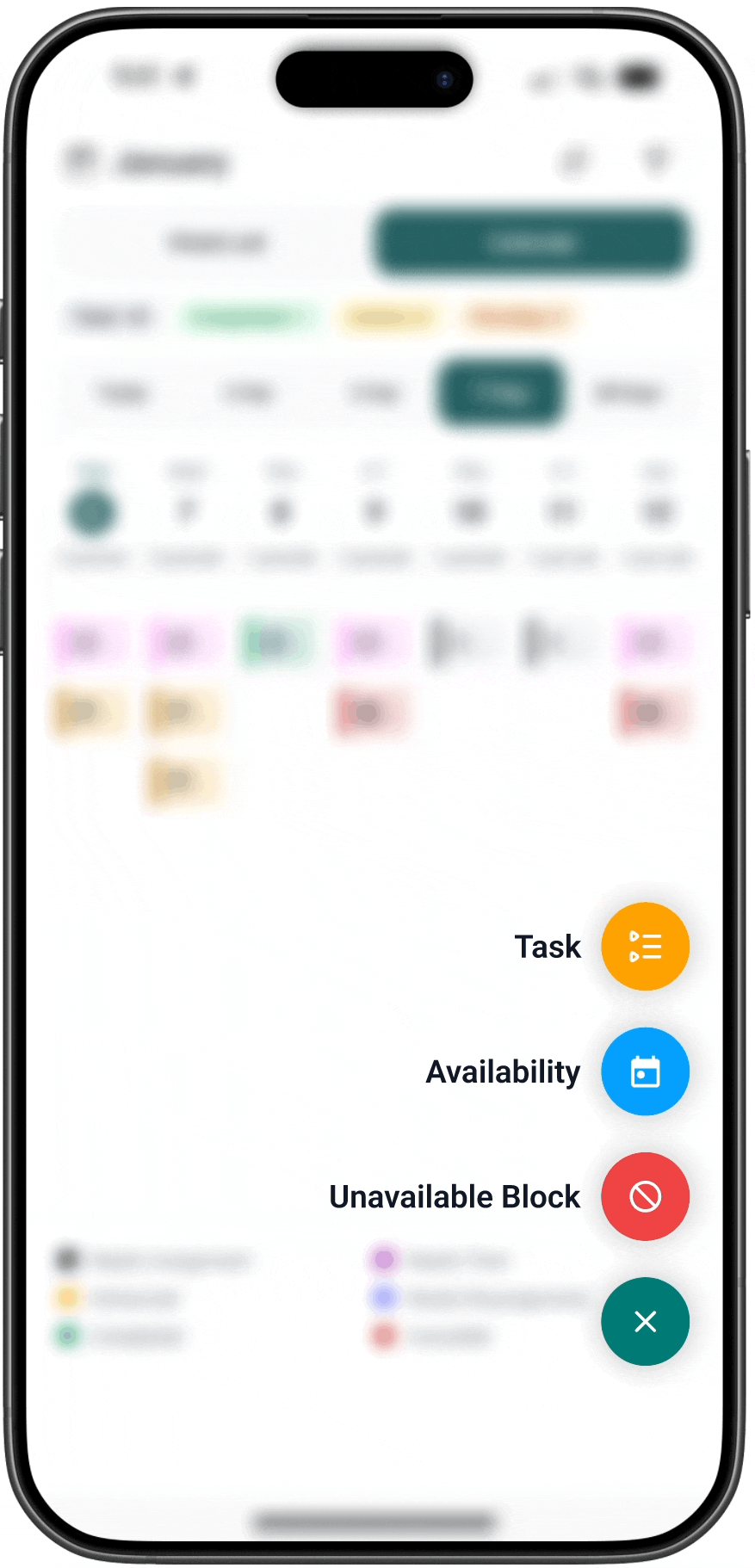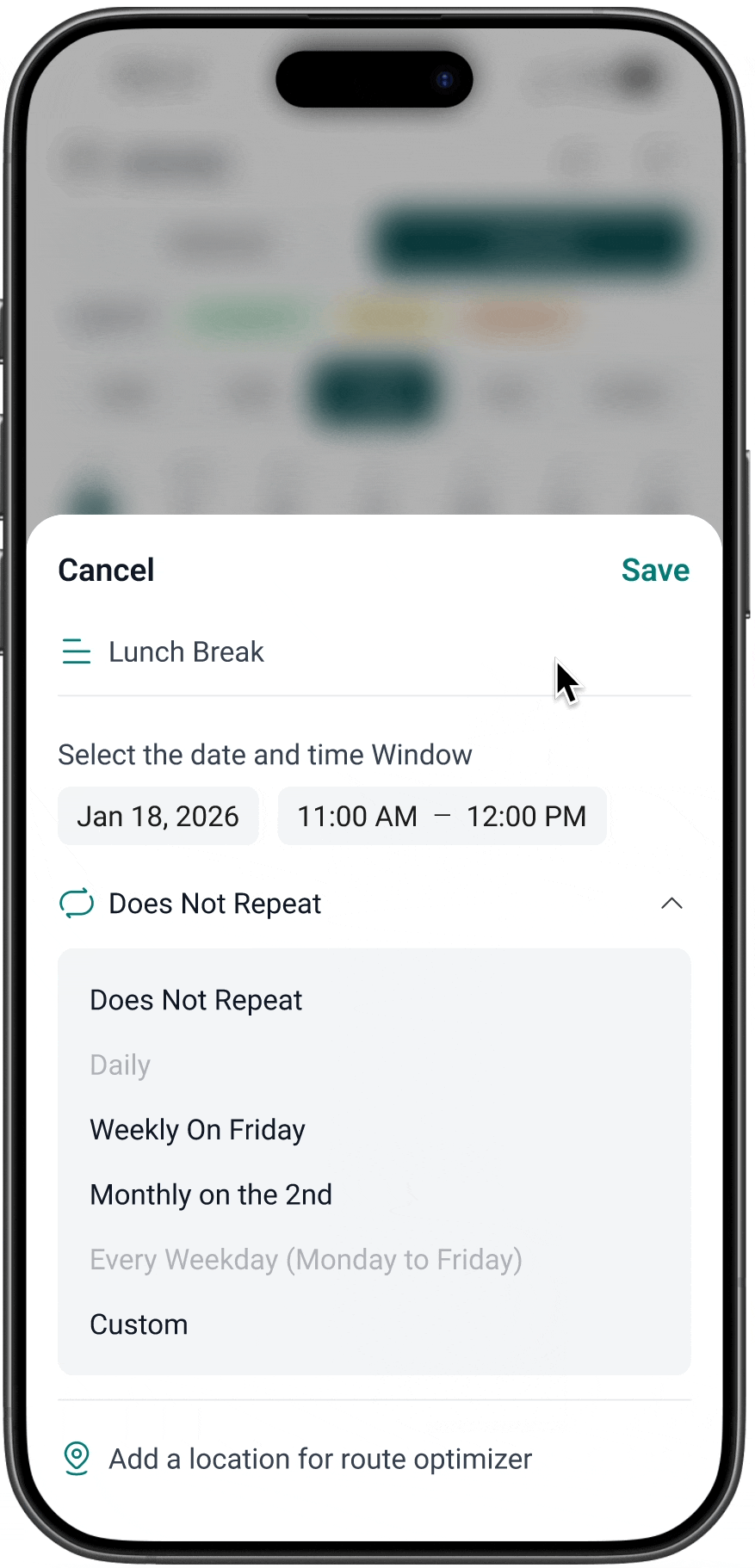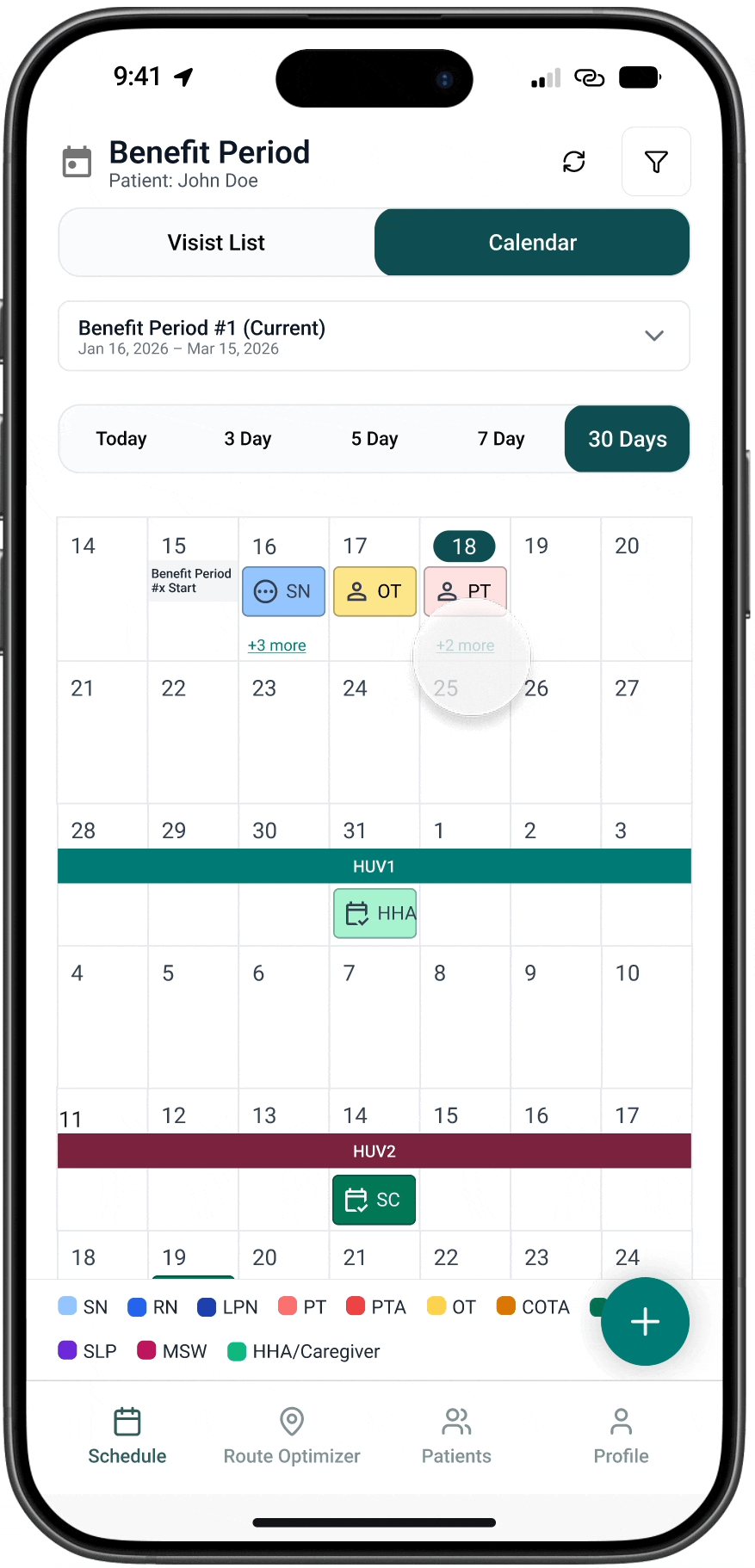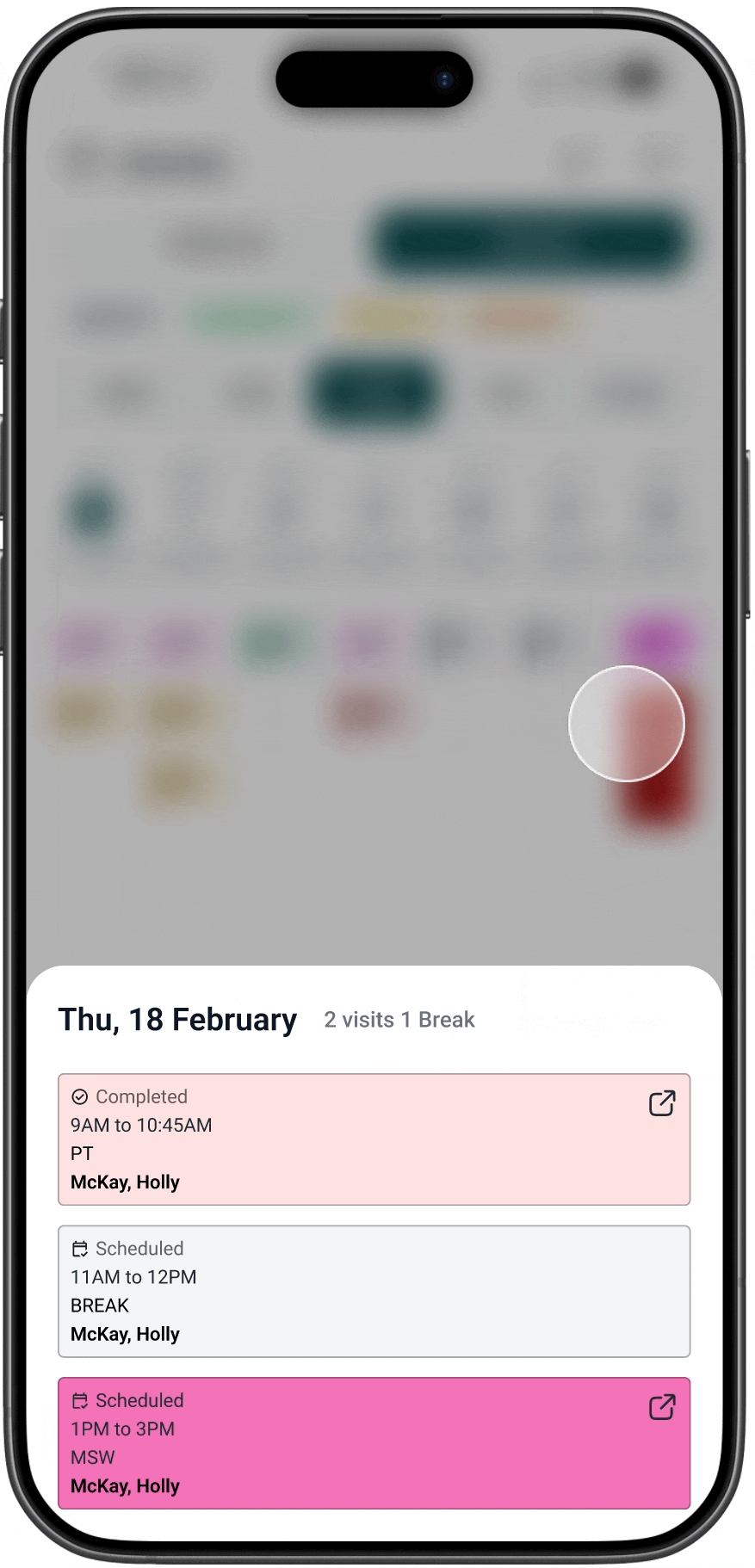
AFTER
01. Coverage timelines are visible
Benefit period boundaries appear directly in the scheduling timeline.

AFTER
02. Eligibility status is surfaced
Visits are automatically classified as eligible or out-of-bounds.

FINAL APPROVAL
The pilot launched at NorthStar Hospital with 3,000+ clinicians. Design was approved after two rounds of stakeholder review with clinical ops, product, and engineering. Weekly cross-functional sessions aligned system rules with real-world workflows before go-live

RESULTS (North Star Hospital Pilot)
Operational Impact
Making Scheduling Constraints Visible
Scheduling is not just a UI surface, it is an operational contract. By making coverage constraints visible at the point of decision, the system reduced ambiguity across scheduling, sales, and onboarding workflows.
Measured through ops signals and workflow review :
-67%
Eligibility verification time
-52%
Manual cross-validation
-25%
Invalid scheduling attempts
+41%
Scheduler confidence
Clarification time dropped from 180 sec to 60 sec, without switching to external records.
Coverage rules surfaced at the point of decision, eliminating the lookup.
Constraint visibility prevented out-of-bound errors before submission.
Confidence score increased from 5.8 to 8.2 / 10, reducing hesitation during scheduling.
WHAT I LEARNED & WHAT'S NEXT
How system design helps clinicians anticipate conflicts before they happen.
01. Constraint visibility changed behavior, not just UI
Making rules explicit shifted schedulers from reacting to errors to anticipating conflicts earlier.
02.The system is still reactive
Conflicts surface after scheduling decisions. The next version should detect constraint violations before submission.
03.Next: Proactive conflict detection
Pattern-based alerts before errors happen — not just faster recovery after they do.